In any case, we checked into Buffalo Children's at 6:00 am on April 9. Nolan was a bit wiped out, but was happy to play the wii in the pre-surgery waiting area.
In the middle of his game, he suddenly sat down and looked quite ill. He said he needed to throw up. We told the nurse and they brought us to a room with a gurney, and called his ENT.
Nolan's stomach is an up-and-down thing.. we've always wondered about hypoglycemia since he vomits more frequently on an empty stomach. They brought us down to the second floor pre-op area, and we waited in the chairs. As Nolan puked his guts up, the anesthesiologist visited with us. The nurse also came and took some blood for a blood glucose reading. His blood sugar was 60, which is at the lower limit of normal for a child. He doesn't have hypoglycemia, so the vomiting is due to some other factor.
In any case, the anesthesiologist saw Nolan's state and told me that I could come into the operating room to be with him while they put him to sleep. I have no idea why they didn't do this for the previous thirteen procedures, but boy howdy - it was so much easier. I walked him back into the OR and held his hand as he drifted off - there was no crying and no hysterics.
After 2 hours, we talked to the ENT for a post-op report. His epiglottis (flap that comes down when you swallow to protect your airway) was flopping over his voice box again, so they tacked that back up. This procedure (tacking the epiglottis to the base of the tongue) is called an epiglottopexy. She also lasered out the floppy tissue (called aryepiglottic folds) that flopped over his voice box. In addition to lasering, she sutured the area to (hopefully) prevent the tissue from collapsing again.
She also told us he has a condition called glossoptosis (gloss-op-toe-sis), which is when the jaw is too small to accommodate the tongue. His tongue falls to the back of his mouth and also obstructs his breathing. If this condition worsens over time, he may need a procedure to fix the problem. Hopefully he won't require help with this issue.
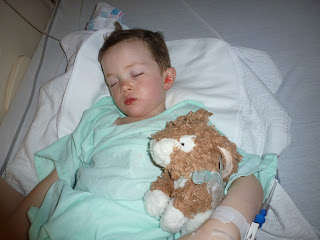
The PICU charge nurse came to retrieve us from the waiting room and brought us to Nolan's bedside. He was heavily sedated and on a ventilator.
Occasionally, he would wake and try to rip the tube from his throat. He was quite wakeful despite heavy sedation - he ended up requiring Fentanyl, Ativan, Versed, and Precedex to maintain a restful state. He did have a fever for the first two days in the PICU, despite the Tylenol they were giving him.
It was a long two days, though at least Nolan was resting comfortably by the second day. His PICU nurse was with him for three days and it was wonderful - his nurse was really amazing and took great care of our little boy. Finally, Thursday arrived and we were able to extubate him.
It took quite some time for the Versed and Remi-Fentanyl to wear off, and our first attempt to take the tube out failed (his O2 sats kept dropping so they left it in for a while). Finally, he woke up enough for the PICU staff to remove the tube. Parents who have gone through this know how heartbreaking it is. Nolan was awake and thrashing, terrified and not really understanding why he couldn't speak. Tears poured silently down his face... the doctors needed Nolan to respond to commands before they could pull the tube. Nolan couldn't do this. There were just silent tears and terror. Finally he mouthed the words, "TAKE THE TUBE OUT." His silent "scream" let the team know he was conscious enough to breathe on his own. They took the tube out.
Once the tube was out, he immediately went back to sleep. His oxygen saturation was great, and we would monitor him for another 24 hours in the PICU. If he could stay awake, eat, and drink, we would be discharged the following day.
Nolan slept all day and did not eat or drink anything. I did not want to stay over the weekend in the hospital. The medical staff wanted to be sure he could drink without choking before sending us home. Fortunately, we talked with the residents and Nolan's ENT - since Nolan has a g-tube, they would allow us to go home despite the lack of eating or drinking.
The following night was really rough. Nolan was very wakeful, but his voice hadn't come back. He would sit up and mouth words, trying to communicate. He couldn't swallow his own saliva, and needed to spit into a towel frequently. Since he was only there for monitoring, his PICU nurse was moved to another patient across the ward and I was the one "on duty" throughout the night.
Friday morning, Nolan woke and was in a great deal of pain - his legs were really bothering him. He gets a strange leg pain every once in a while - not exactly cramps, but he will yell at us to crush his toes, pull on his leg, and pull his feet off. I have no idea what causes this, but I was glad that other medical personnel saw this! Nolan felt very poorly, and we were discharged at 11:00 to go home. I was beyond tired, and grateful to get home.
The leg pain continued for the rest of that day, and was actually more difficult than anything else. He writhed on the floor yelling, "PULL MY TOES OFF!!!" There was really nothing I could do to help him - fortunately the episode passed after a few hours and he was fine later that evening.
Nolan can't swallow liquids well, so he coughs and splutters frequently with drinks. We are putting liquids through his tube. Fortunately, he can eat some foods. Cheese puffs, pancakes, and other dissolvable foods work well. He tried a bite of pizza, but ended up spitting it out. He can't do any "hard" foods like apples or chewy bread. He's still spitting out his saliva - but this should get better over the next few days.
His low-grade fever has made a bit of a comeback, but each day is better than the last. We have even seen a smile or two over the past day or so. I'm not sure when he can return to school. He is far too ill at the moment to do anything, and the choking problem has to be resolved before he can return safely to his classroom. It will probably be another couple of weeks before he's well enough to return to regular activities.
A small smile.







4 comments:
Thanks for the news - you must be exhausted.
Praying for healing, comfort, and peace,
Julie
Thinking of you guys...hoping for quick healing and a happy little boy!
He's doing really well now - almost back to normal! Still choking on thin liquids, but otherwise doing well. He'll be back to school on Monday, I think!
I just ran across this! My son had a superglottoplasty about 15 months ago. His stridor improved but his constent illness and chocking didn't get better. In july 2012 he had a largygeal cleft repair. This almost immediatly fixed the choking and low o2. However, the last 6 weeks his stridor has came back and is getting worse. We see the dr. Next week. He also has some choking that came back but it is still 80% better than before surgery (I think it is beciz his throat is sore from stridoring). Anyway, you have said that your son is still choking. ....have the doctors checked to see of he has a laryngeal cleft?
Post a Comment